When we last left off in our tale, our dynamic protagonist got her time slot scheduled for VSG weight loss surgery.
So the morning of… my big day. I didn’t sleep well the whole night before. I packed and re-packed my hospital bag a few times, and thought about what I would wear to the hospital and what I’d wear back home for maximum comfort and ease if I was sore or was in pain. The morning of, I woke up at 5:30 am to be out of the house by 6:30 to be at the hospital for my 7:30 am reporting time. I’d settled on wearing a stylish Mickey Mouse pajama set I’d gotten from Avon. I packed an old Jujube diaper bag as my hospital bag with a few things – phone charger, socks, slippers, going home outfit, some toiletries and my contact lenses. It was explained that I could not wear contacts during surgery so I wore glasses on the morning-of. Here’s my spiffy Day-Of/Before Photo:

And just like that we were off. I let Mike drive us to the hospital since I was tired and nervous. Since I wasn’t driving, it gave me a chance to start my Snapchat surgery story.

Arrived at the hospital and did all the administrative check-in procedures asked of me. Then the medical check-in procedures like blood and pee in a cup. And laughed and laughed and laughed when they asked me “could you be pregnant.” Super nope, how dare you, get that trash talk away from my good vibes. I got into my weird gown that had a hole in it for an air tube that blew hot air at me to keep me warm, and honestly? I’m into it. I’d like that for home. Next, the anesthesiologist came in to speak with me and go over things about me and my health and asked me if I had any questions, and I asked a basic moron question like “what are the odds of someone not waking up from anesthesia randomly?” and the odds were pretty low. But he was kind and patient and didn’t call me a fucking moron so that was cool. Then it was time for surgery and my surgeon, resident and crew were wheeling me away.
And that was that, I was in the operating room, moved over to their table from my bed, was starting to get nervous as they started preparations around me. It was a large, bright white room and very well-organized. Everyone in there knew what they were doing like a well-oiled machine. Then it was anesthesia time and the next thing I know, I’m waking up in recovery.
Recovery was a weird place. I woke up very groggy, in pain, and nauseous as hell. Some woman came over and was doing touch-assist pain relief of some kind. I had honestly completely forgotten about that and chalked it up to being a weird dream, until I saw it happen when my boyfriend had his surgery months later. They send the touchy-lady over to do some kind of healing/comfort maneuvers on you until your pain meds or whatever meds kick in or are ordered. My order was delayed for some reason so I’m like ugh please don’t let me puke on this nice lady who’s touching me. When I stressed to the nurse I needed relief, that I felt like the hottest garbage in an August dumpster, she gave me pain medication, as well as an anti-nausea patch Scopolamine. That shit worked almost instantaneously. It was amazing and I was so grateful for the relief and the relentless caring I received in the recovery unit. The patch is worn for about 72 hours, and I’d never experienced any further nausea after the patch.
Within an hour or two after I was deemed stable in recovery, I was moved into my own private hospital room. The hospital I was in has a specific floor dedicated to bariatric surgical care. So the staff on that floor is all very well-versed with the care and needs of the people having weight loss surgery. It was explained to me that to be most successful and have a healthy recovery, I should be up and walking as soon as possible. They even gave me a little pedometer clipped to my sock to see how much I was walking, instead of just taking my word for it that “yeah sure I’m walking.” I’m not going to sugar coat this, but I had never felt so fatigued and run down in my life. I didn’t want to get out of bed at all. That first afternoon I took one or two slow, tiresome walking laps around the unit my room was located in. But I honestly did not want to do anything. Not out of laziness, but I would come to see that my blood pressure was CRAZY low. The nurses kept asking me “hey do you feel ok???” and I was like “yeah I’m just so tired…” staying awake required way more focus and stamina than I could muster up. By the next morning I was feeling more alert and my BP was creeping back up to a more normal range, but that first night I was a little worried that there might be something wrong with me.
First thing the following morning they sent me for a swallow-test. This was done in the radiology imaging department. I was given some kind of drink that they told me to take sips of as they watched it go down my throat via imaging or x-ray, and then land in my stomach and make sure there was no leaking from my stomach staples inside. Once I passed my test, I was allowed to have my first post-op “meal” …which, frankly, I didn’t even want except for being very thirsty. This was all clear liquids – diet lemonade drink, chicken broth, sugar free jello and water.

This “meal” would be all that I was allowed to have for the following two weeks, with the addition of 2oz of a protein shake 3 times per day. And this was fine. I sincerely and truly was not hungry. It was like I woke up with that part of my brain removed or something. I did not care about food at all, I was not dissatisfied for the sad liquid meals I was forced to have. It was a relief, honestly, for the first time in my life to not be preoccupied with my food, what I was going to eat next, or any of it. After the doctor and nurses observed that I could eat my liquid-meal with no adverse effects, I was discharged and sent home. So from check-in to discharge, I spent about 32 hours in the hospital all together.
So another awesome perk about this surgery besides all the wonderful life-altering things about to happen to me, was that I got liquid vicodin to take for the pain. I will not lie, I can totally see how and why people get addicted to painkillers. This stuff is amazing. Warm & tingly & pain free. I wasn’t in too much pain, thankfully, but the medication helped a lot. It helped me be able to get up and move around and all together recover more quickly. By my third day home, I went out for a walk in the park… did a mile, and felt pretty worn out, but was glad that I was able to do something. I was going to have to figure out how I’d work fitness into this new lifestyle, and walking is a decent start.
I had scheduled my surgery on a Thursday of a long weekend, and had planned to be back in work the following Wednesday if I felt ok. And I did! It was really an easy recovery and I feel like I handled it well. I brought my vicodin to work to take after I arrived so I would not be under any influence while driving.
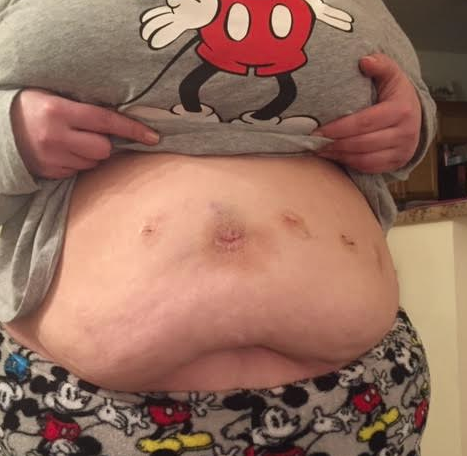
One hard part about recovery? My surgical incisions were quite itchy. I might have been low-key allergic to the surgical glue used to close my skin up. Here’s what my incisions looked like the next day at home. Bruised, red and weird. They healed very nicely now, and it’s hard to even find the scar at this point. I’ll have to take a photo at some point (for part three…) to show that off I guess. There were five incisions all together and I used Bio-Oil on them after they healed slightly to reduce whatever scarring might occur. The rest of my two weeks would be spent just doing my thing – working, living, drinking tiny amounts of Premier Protein and biding my time till my first post-op appointment. At the next appointment, I’d be given the clearance to advance to the next step of my diet. And though I’d stated this was the first time I didn’t care about food, after 14 days of no actual food, I was starting to feel a little weird about things. The mind needs food as much as a body does. Not chewing on things for an extended period of time is weird. I started to get cranky. I knew that the next phase of the diet was soft foods, soups, eggs, yogurt… and I was eager for that to begin.

After my two-week, then six-week follow-ups, I was progressing just as I should. Little by little, each week added in new forms of food – first soft foods, then soft protein like fish and seafood the following week. I am not a person who likes fish or seafood, but I tried out some shrimp just to see. It was alright, but I haven’t tried it since so it’s not really something that’s making its way into my routine whatsoever. Then came more firmer proteins like chicken, pork and beef. Each step of the way I was doing just fine, nothing tripped me up, there was no nausea. Once or twice I’d eat a larger amount than I should have and immediately regretted it by having sharp stomach pains for about half an hour. The only cure for me was to lay down till that subsided. But it’s a whole new way of eating, so there was bound to be some lessons learned along the way. To this day there are foods that just don’t sit well – I can eat sugar just fine, breads, I can eat like normal foods like a normal human, just in smaller amounts. But for whatever reason, rice and oatmeal do not make me feel good at all.
This wraps up Part Two. Stay tuned shortly (and I mean it, like in a few days, not in a month) for Part Three on Putting In The Work.
One Response to “Keeping it 100 (part two)”
Keeping It 100 (part three) – Night Caffeine
[…] Read Part 2: Getting Surgery here […]